E-newsletters
November 2021: Lung Ultrasound – The Missing Clinical Piece

Respiratory related pathology are some of the most common yet vexing complaints that have to be dealt with in the primary care setting. The differential diagnosis is broad, ranging from infectious pathology to underlying cardiac and pulmonary disease. And when considering the global community, the list gets even broader and more puzzling by having to consider diseases such as tuberculosis and environmental exposures such as asbestos that can occur at a higher prevalence.
Typically the clinical decision making and medical management involve lab work and imaging to look for signs of infection or alternative explanation such as cardiac disease or anemia. More than anything, the work up is delayed as the majority of the imaging and lab work cannot be performed and resulted instantaneously. But that is where Lung Ultrasound and POCUS can play the differentiator!
Lung Ultrasound
Lung Ultrasound is an established and highly utilized component of POCUS. The wealth of knowledge that can be acquired with a few quick views and settings is also critically important to the clinician to help establish a medical decision making process for a variety of chief complaints including shortness of breath, chest pain, and weakness. It can be applied to assess for a variety of abnormal physical exam findings such as tachycardia, tachypnea, respiratory distress, hypoxia, and fever. If trauma is a component of the clinical history, then lung ultrasound can help with identifying critical findings such as hemo or pneumothorax.
GUSI is a Global Leader in Teaching Lung Ultrasound
Utilizing Lung Ultrasound in coordination with other POCUS exams helps to develop a complete evaluation of the patient. This has been even more relevant since the onset of the COVID-19 pandemic, primarily resulting in pulmonary related symptoms.
Here are two examples of how POCUS with Lung Ultrasound was pivotal in changing the course of management for patients, which is highlighted in our new Local Heroes Series:
|
Case Study #1 69yo male, with a history of leprosy currently undergoing treatment, as well as long-term smoking, presented to clinic at a small government hospital in Lusaka, Zambia, with a chief complaint of lower extremity edema, which over the last few months progressed from the feet/ankles up to his thighs and genitalia. He had not seen a clinician for as long as he could remember. Other than some dyspnea on exertion and orthopnea, the remainder of the review of systems was negative. Significant findings on physical exam included significant barrel chest, 2+ systolic murmur on cardiac auscultation, diminished breath sounds throughout all lung fields with significant bibasilar crackles, and 3+ edema of the lower extremities bilaterally to the level of the scrotum, penis, and lower pelvic wall. See the POCUS clips below: 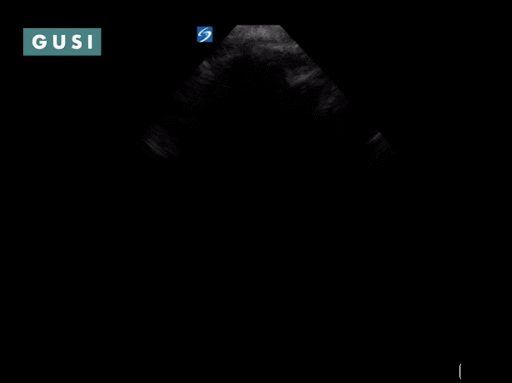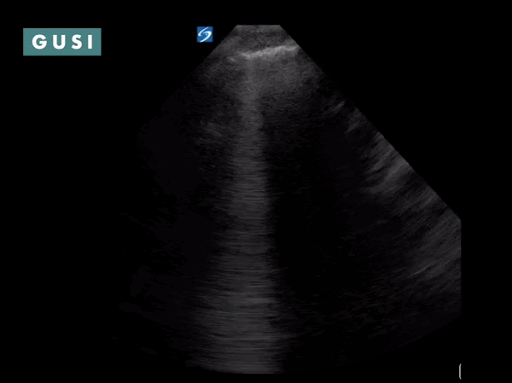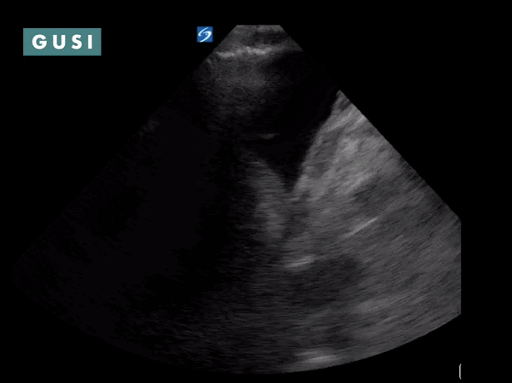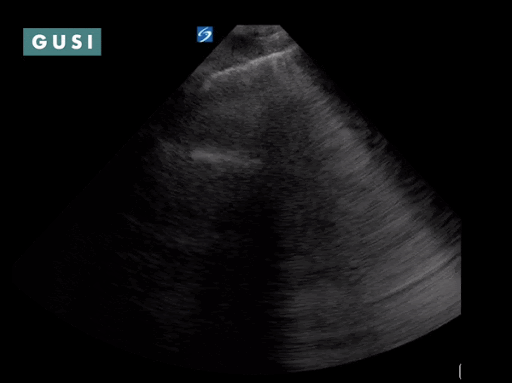 Lung Views showing Pleural Effusion and B Lines 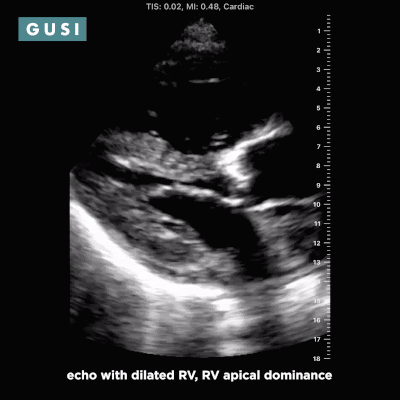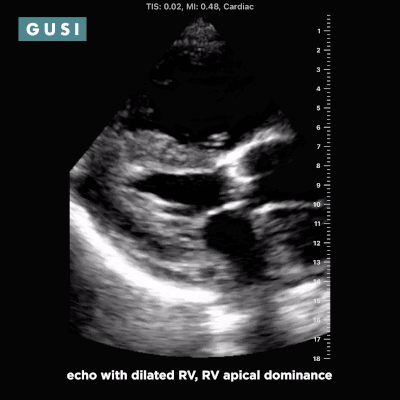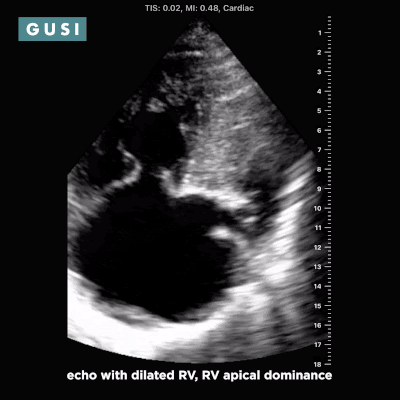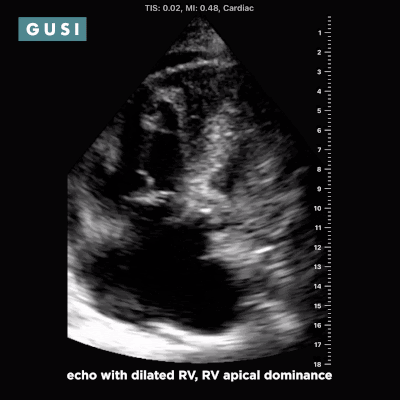 Echo with dilated RV, RV apical dominance 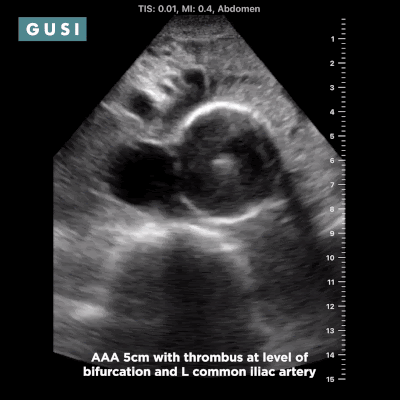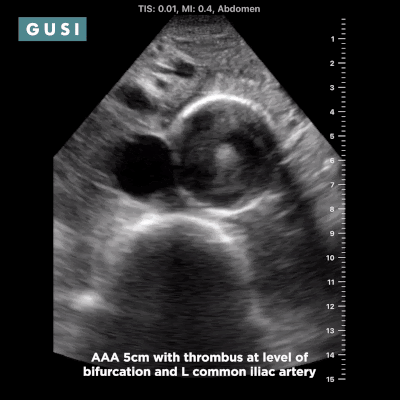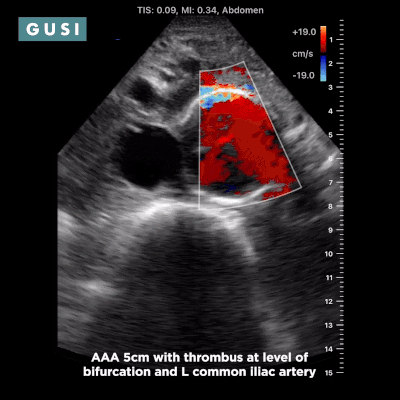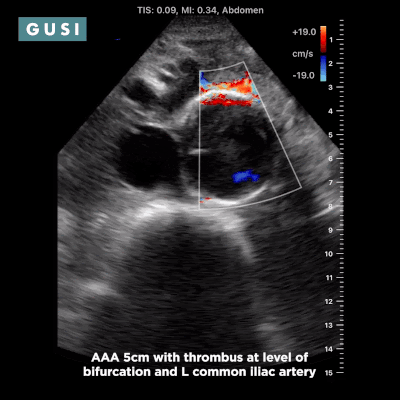 AAA 5cm with thrombus at level of bifurcation and L common iliac artery POCUS helped determine the diagnosis of R-sided heart failure likely secondary to cor pulmonale from long standing COPD, as well as a completely unexpected and unanticipated AAA requiring immediate vascular surgery evaluation. While the initial plan was to admit the patient to the local hospital for diuresis and heart failure management, these POCUS findings of AAA prompted immediate referral to Lusaka’s tertiary center for urgent vascular surgery consultation in addition to the medical management of his other conditions. POCUS in the clinic significantly changed the clinical course for the patient and resulted in finding and addressing the urgent findings of AAA. * Thank you Dr. Matthew Haldeman |
|
Case Study #2 37yo old male with a history of smoking presented to urgent care in Northern California with 3 days of shortness of breath and generalized malaise. He denied fevers, chills, chest pain, leg swelling. His vital signs were remarkable for a HR of 110, RR of 24, T 98.6 and O2 sat of 90% on room air. His lung exam was difficult to obtain because the patient was in an isolation room awaiting testing for COVID and the air filtration unit in the room was very loud. The patient was immediately placed on oxygen by nasal cannula and a bedside lung ultrasound was performed revealing the following findings: Left hemithorax chest shows normal A line pattern and normal lung sliding present. Right hemithorax shows the following: 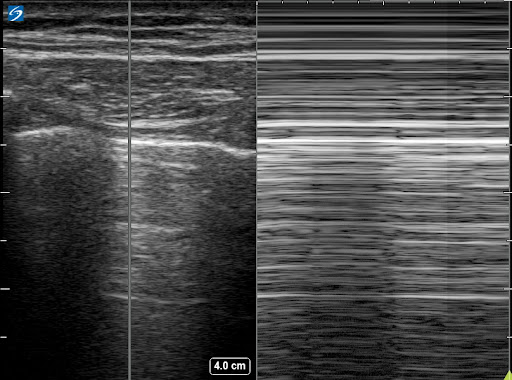 Absent lung sliding is represented in M Mode as the “stratosphere” or “barcode” sign. The presence of the lung point is the most specific finding in a pneumothorax. The lung point is the location at which the lung re-expands from a pneumothorax represented by the point that separates the presence and absence of lung sliding. In this patient, an x-ray confirmed the presence of a pneumothorax. However, the absence of a pneumothorax on CXR did not rule out the presence of a pneumothorax given the lower sensitivity of chest x-ray to diagnose pneumothorax. According to the study by Ding et al in CHEST, the pooled sensitivity for chest x-ray to diagnose pneumothorax was 0.52 and 1.00 compared with .88 and .99 for ultrasound, respectively. The patient had a thoracic vent placed and did well. His COVID test returned negative. Ultrasound in this case led to an immediate rapid diagnosis of Pneumothorax and appropriate management of this life-threatening pathology. |
|
Highlighting our POCUS Training Courses in 2021 GUSI held our POCUS in-person training course over a two day period in October 2021 in San Francisco. We were able to train over 30 healthcare providers in various aspects of image acquisition, interpretation, and application in the clinical setting. We all learned from this experience and gained critical skills for the betterment of our patients. We were proud to be able to safely hold in-person courses over the year in 2021, in addition to the San Francisco course. In these courses, over 95% of the students surveyed afterwards said that they felt more confident in their POCUS skills after the course and that they would apply these skills in the clinical setting. In November 2021, GUSI also supported the first ever training course in Zambia – POCUS for the Zambian Clinician: An Introduction to Bedside Ultrasound. The course was held in collaboration with the Association of Family Physicians of Zambia (AFPAZ) and took place at Kanyama Hospital in Lusaka, Zambia with efforts spearheaded by Dr. Matthew Haldeman.  POCUS for the Primary Care Provider, San Francisco, California  POCUS for the Zambian Clinician: An Introduction to Bedside Ultrasound, Kanyama Hospital in Lusaka, Zambia. POCUS Training is for Everyone Future 2022 POCUS in-person training courses will include our Introduction to POCUS Course for Physician Assistants January 2022 at Samuel Merritt University.
|
GUSI News & Updates
Are you a clinician who provides care in low- or middle-income countries or other low-resource areas? POCUS can transform how you provide care! We invite you to join our growing community of global ultrasound practitioners. GUSI offers a variety of online and in-person courses that can guide you from little to no POCUS knowledge to a level of mastery in any clinical setting.
Coming Soon!
Our website will soon host exciting and educational content around POCUS in the setting of Critical Care, Pediatrics, and Musculoskeletal and Sports Medicine!
Learn more here.
|
Health Equity Residency Exchange (HERE) The Health Equity Research Exchange (HERE) program is the latest way that GUSI is living up to its promise to share POCUS with medical professionals from around the world. For every resident who signs up to learn with GUSI, we will extend a full scholarship to a resident practicing in a low- or moderate-income country.
Learn more and sign up to participate at https://bit.ly/GUSI_HERE |
|
links to https://globalultrasoundinstitute.com/
“Jelly Squad” POCUS interest group at the Swedish First Hill Family Medicine Residency learning POCUS with GUSI. |
Sign up for GUSI’s e-newsletter and updates here.





