E-newsletters
June 2021: Why POCUS is a Game Changer in Global Health

It is estimated that in approximately 25% of all medical cases worldwide, clinical considerations alone are not sufficient to make a correct diagnosis. Unfortunately, according to the World Health Organization, two-thirds of the world’s population live in areas without easy access to diagnostic imaging. As clinicians, how can we bridge this resource gap to ensure that every patient—regardless of where they call home—has access to diagnostic imaging and, ultimately, the highest quality care?
The answer is point-of-care-ultrasound (POCUS).
As a handheld, affordable, and versatile imaging modality, POCUS plays a critical role in global health settings. POCUS rapidly narrows differential diagnoses at the bedside in minutes; enables safer and more accurate ultrasound-guided procedures; and empowers clinicians to put the diagnostic process entirely in their own hands. Multiple studies have shown that POCUS can change the clinicians’ diagnosis and plan one-third of the time or more.
Here are two examples of how POCUS enhances the delivery of high-quality care in low-resource settings around the globe:
|
Case Study #1 A 79-year-old Zambian woman presented to a family medicine clinic complaining of right upper quadrant abdominal pain and distension. Progressive abdominal distension, now her right upper abdomen bulges out significantly. She denied weight loss, night sweats, or fever. Pre-POCUS ddx includes hepatocellular carcinoma or amebic liver abscess.
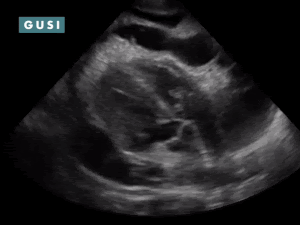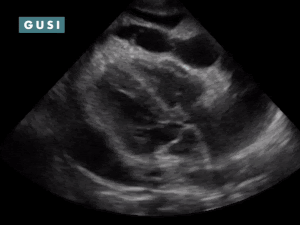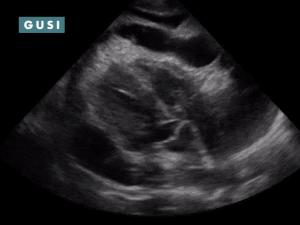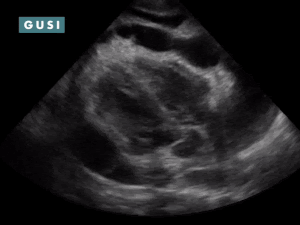
POCUS Findings: Massive anechoic liver cyst in the right liver lobe, obliterating most of liver parenchyma, with several smaller cysts in the left liver lobe. Hypoechoic material is noted in the gravity-dependent portion of the cyst—suspicious for hydatid sand. Scattered hyperechoic debris is also noted in the cyst lumen with patient position changes— “snowflake” sign. No internal septations or germinal wall layer detachment (“water lily sign”) is noted. POCUS-Assisted Diagnosis: The clinician now suspects a large hydatid cyst in the right liver lobe, likely stage CE1 (active). Subsequent assessment included determining whether it is a large simple cyst or a malignancy. The follow-up plan included: 1. Serologies for Echinococcus granulosus ordered. 2. Albendazole course initiated. 3. Referral to general surgery completed for consideration of PAIR procedure vs. surgical excision. * Thanks to Dr. Matthew Haldeman for sharing this case study from Zambia. |
|
Case Study #2 A 61-year-old patient with a history of DM2, HIV, and CRI on dialysis who presented with new shortness of breath, easy fatigability, and swelling was overdue for dialysis. The patient also had a dry cough and weight loss for two months. Hypotensive, tachypneic with increased effort, decreased breath sounds, and dullness to percussion in lower lobes.
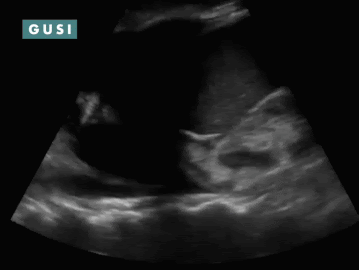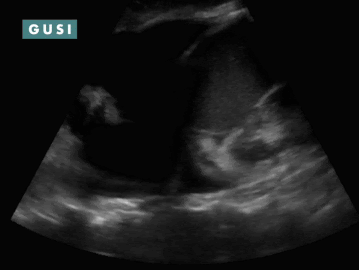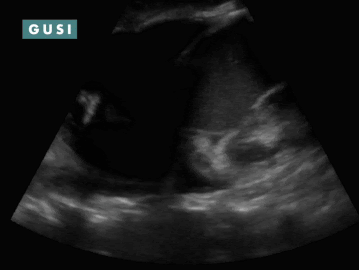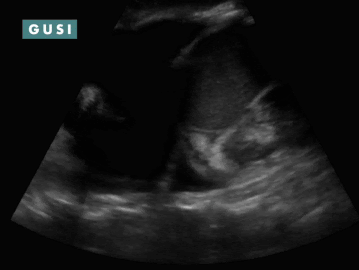
POCUS Findings: 1) Bilateral moderate-sized pleural effusions (anechoic fluid in thorax superior to diaphragm; spine sign: visibility of thoracic spine above the diaphragm in the thorax and loss of mirror artifact over diaphragm. 2) Chronic-appearing pericardial effusion with fibrinous stranding classically seen in effusions from tuberculosis. No clear evidence of pericardial tamponade (no RA systolic collapse, no RV diastolic collapse, and no sonographic pulsus paradoxus) or constrictive pericarditis. TB pericarditis is diagnosed. Course: Patient was admitted, found to be coagulopathic, had his coagulopathy reversed, was dialyzed, had hyperglycemia controlled, and underwent a diagnostic pericardiocentesis which was positive for TB. He was initiated on TB therapy as well as HAART. The patient improved, was discharged, but ultimately was non-compliant with his medications due to difficulty accepting the HIV diagnosis and unfortunately had a poor outcome. *Thanks to Dr. Romeo Wahome for sharing this case from Kenya. |
|
“POCUS in Global Health” Webinar To see more POCUS cases in global health settings, check out this webinar from the POCUS Certification Academy featuring GUSI co-founder Dr. Kevin Bergman, GUSI instructors Drs. Nahreen Ahmed and Kaya Belknap, and other experts:
|
Are you a clinician who provides care in low- or middle-income countries or other low-resource areas? POCUS can transform how you provide care! We invite you to join our growing community of global ultrasound practitioners. GUSI offers a variety of online and in-person courses that can guide you from little to no POCUS knowledge to a level of mastery in any clinical setting. Learn more here.
GUSI News & Updates
|
POCUS for Primary Care Live Course in San Francisco October 21 – 22, 2021 Registration for our in-person POCUS course is open now! This acclaimed, CME-accredited course combines high-yield focused lectures and loads of hands-on scanning sessions with skilled POCUS mentors and educators. The MSK portion on day 2 will be taught by Dr. Ryan Petering, noted MSK educator and Director of the Sports Medicine Fellowship at Oregon Health Sciences University. In addition, participants receive one year of complimentary access to our online Essentials Course in POCUS (25 CME hours). Learn more and register here. |
|
Launch of the Health Equity Residency Exchange (HERE) The Health Equity Research Exchange (HERE) program is the latest way that GUSI is living up to its promise to share POCUS with medical professionals from around the world. For every resident who signs up to learn with GUSI, we will extend a full scholarship to a resident practicing in a low- or moderate-income country.
Learn more and sign up to participate at https://bit.ly/GUSI_HERE |
|
Bringing POCUS to Rohingya Refugee Camps GUSI and MedGlobal have been awarded the 2021 MissionPOCUS grant from POCUS Certification Academy! Together we will train physicians in the Rohingya refugee camps in Bangladesh to use POCUS. Learn more here.
|
Sign up for GUSI’s e-newsletter and updates here.